Allergic Endotypes in Biologic Prescribing: The 2026 Guide for UAE Labs
As the UAE healthcare landscape evolves toward the 2031 vision of precision medicine, the clinical management of severe asthma and allergic disease is undergoing a fundamental shift. For years, clinicians relied on phenotypes; the observable characteristics of a disease, to guide treatment. However, in 2026, it is becoming increasingly clear that two patients with the same “severe allergic asthma” phenotype may respond very differently to the same biologic therapy.
To achieve better clinical outcomes and satisfy the rigorous requirements of modern insurance reimbursement in Dubai and Abu Dhabi, we must look deeper. We must move from phenotypes to allergic endotypes. This blog explores the critical role of molecular mapping in identifying these biological pathways, the necessity of precision diagnostics for biologic eligibility, and how advanced tools are streamlining the transition from generalized care to targeted therapy.
Defining the Shift: Phenotypes vs. Endotypes
A phenotype describes what we see: a patient with frequent wheezing, high rescue inhaler use, and perhaps a history of atopy. An endotype, conversely, describes the functional and pathobiological mechanism that causes those symptoms.
In the era of targeted biologics, treating a phenotype is like trying to fix a car engine by only looking at the smoke from the exhaust. Treating an endotype is like plugging in a diagnostic computer to find the exact sensor that failed. For specialists in the GCC, identifying these specific pathways is no longer a luxury; it is a clinical necessity for biologic prescribing.
The 2026 Standard for Biologic Prescribing
The biologics available today, such as anti-IgE, anti-IL-5, and anti-IL-4/IL-13 therapies, are highly specific. Their efficacy depends entirely on whether the patient’s underlying inflammatory driver matches the drug’s mechanism of action.
- Anti-IgE (Omalizumab): Primarily targets the IgE-mediated pathway.
- Anti-IL-5 (Mepolizumab, Benralizumab): Focuses on eosinophilic inflammation.
- Anti-IL-4/IL-13 (Dupilumab): Blocks the shared receptor for cytokines driving T2-high inflammation.
If a clinician prescribes an anti-IL-5 biologic to a patient whose severe asthma is driven by a non-eosinophilic endotype, the treatment will likely fail, leading to “diagnostic leakage”, the clinical failure to correctly identify a condition (misdiagnosis), and wasted healthcare resources. This is why allergic endotypes in biologic prescribing has become the primary focus for UAE lab managers and pulmonologists.
Why Phenotypes Fall Short in Precision Medicine
Phenotypes are often “noisy.” A patient might present with an allergic phenotype due to environmental triggers in the UAE, such as desert dust or AC mold, but their internal endotype might actually be “T2-low” or neutrophilic.
Relying on observable traits alone can lead to several clinical pitfalls:
- Ineffective Treatment Cycles: Patients may spend months on expensive biologics that do not address their specific molecular driver.
- Insurance Denials: In 2026, UAE insurers increasingly demand “molecular proof” of an endotype before approving high-cost therapies.
- Incomplete Remission: Without targeting the root mechanism, the patient may achieve symptom relief but continue to suffer from underlying airway remodeling.
The Role of MADx Molecular Allergy Testing
To bridge the gap between “what we see” and “what is happening,” advanced diagnostics are required. This is where MADx molecular allergy testing becomes a transformative tool for the modern laboratory.
Unlike traditional extracts that provide a broad overview of sensitization, the MADx ALEX3® platform utilizes Component-Resolved Diagnostics (CRD). By testing for 295+ allergen components and total IgE simultaneously, it allows clinicians to map the exact molecular profile of a patient’s sensitivity.
Identifying the “T2-High” Endotype
The most common endotype in severe asthma is T2-high inflammation. This pathway is characterized by elevated IgE and eosinophil counts. Using MADx molecular allergy testing, clinicians can confirm if a patient’s T2-high status is truly IgE-mediated. This distinction is vital for deciding between an anti-IgE biologic and an anti-IL-4/IL-13 biologic.
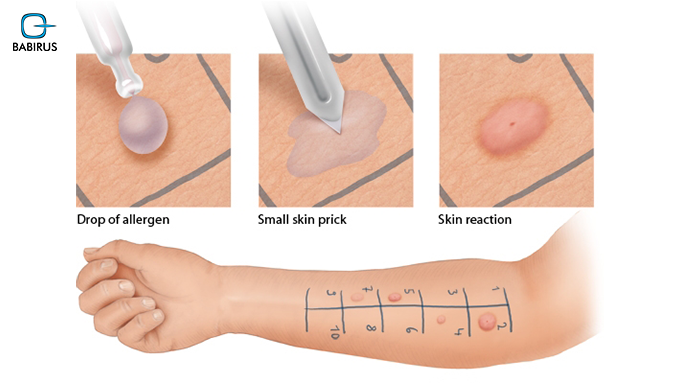
Eliminating Cross-Reactivity Confusion
Traditional skin prick tests or extract-based blood tests can show “false positives” due to cross-reactive proteins like profilins or PR-10. MADx technology includes powerful CCD (Cross-reactive Carbohydrate Determinants) blockers, ensuring that the results reflect true sensitization rather than irrelevant cross-reactivity. This precision is essential when establishing the clinical justification for a specific biologic endotype.

Increasing Insurance Approval Rates for Biologics in the UAE
The financial landscape of UAE healthcare is more scrutinized than ever. With the integration of genomic and diagnostic data into platforms like Malaffi, there is a “digital trail” for every clinical decision.
For a hospital or private clinic, the business potential of utilizing endotype-based diagnostics is clear. By using MADx molecular allergy testing to prove biologic eligibility, providers can:
- Increase Approval Rates: Presenting an insurer with a comprehensive molecular map of a patient’s endotype makes a “denial” much harder to justify.
- Improve Patient Retention: Fast, accurate results lead to “Day 1” precision, preventing patients from seeking second opinions at competing facilities.
- Optimize Lab Throughput: Automated platforms like those provided by MADx allow for high-throughput testing with minimal hands-on time, a critical factor for labs facing staffing shortages.
Moving Toward “Theratypes”
The ultimate goal of endotyping is the creation of a “theratype”, a prediction of treatment response based on the patient’s unique biological pathways. When a clinician in Dubai or Abu Dhabi orders a molecular panel, they are no longer just asking “is this patient allergic?” They are asking “which biologic will provide the highest probability of remission?”
This shift is particularly relevant for the pediatric population. Early endotyping in children can identify the “Allergic March” before it progresses to severe, irreversible asthma. By intervening with the right biologic at the right time, we can fundamentally change the trajectory of a patient’s life.
Conclusion,
In 2026, the term “Allergy” is being replaced by a more nuanced understanding of molecular interactions. For Babirus, the mission is clear: provide the tools that turn clinical suspicion into molecular certainty.
By moving beyond phenotypes and embracing allergic endotypes in biologic prescribing, the UAE healthcare community is setting a global standard for excellence. Whether it is through the deployment of the MADx ALEX3® system or the integration of AI-driven interpretive software, the focus remains on the individual patient.
The era of “one size fits all” is over. The era of the endotype has arrived.
